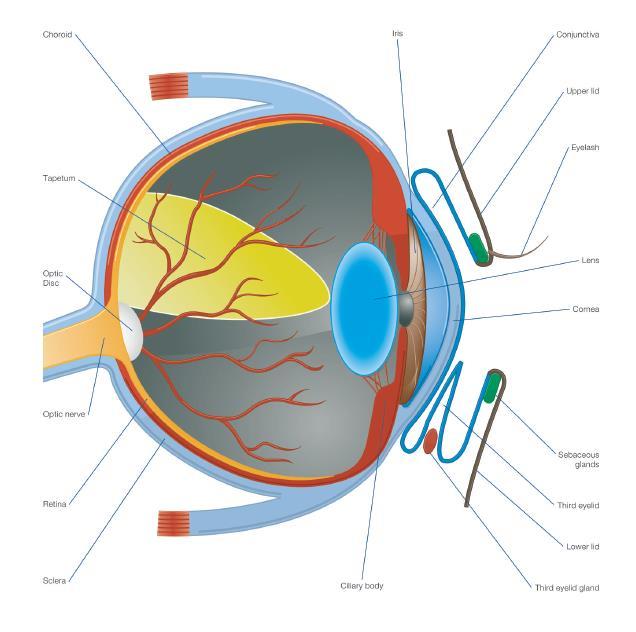
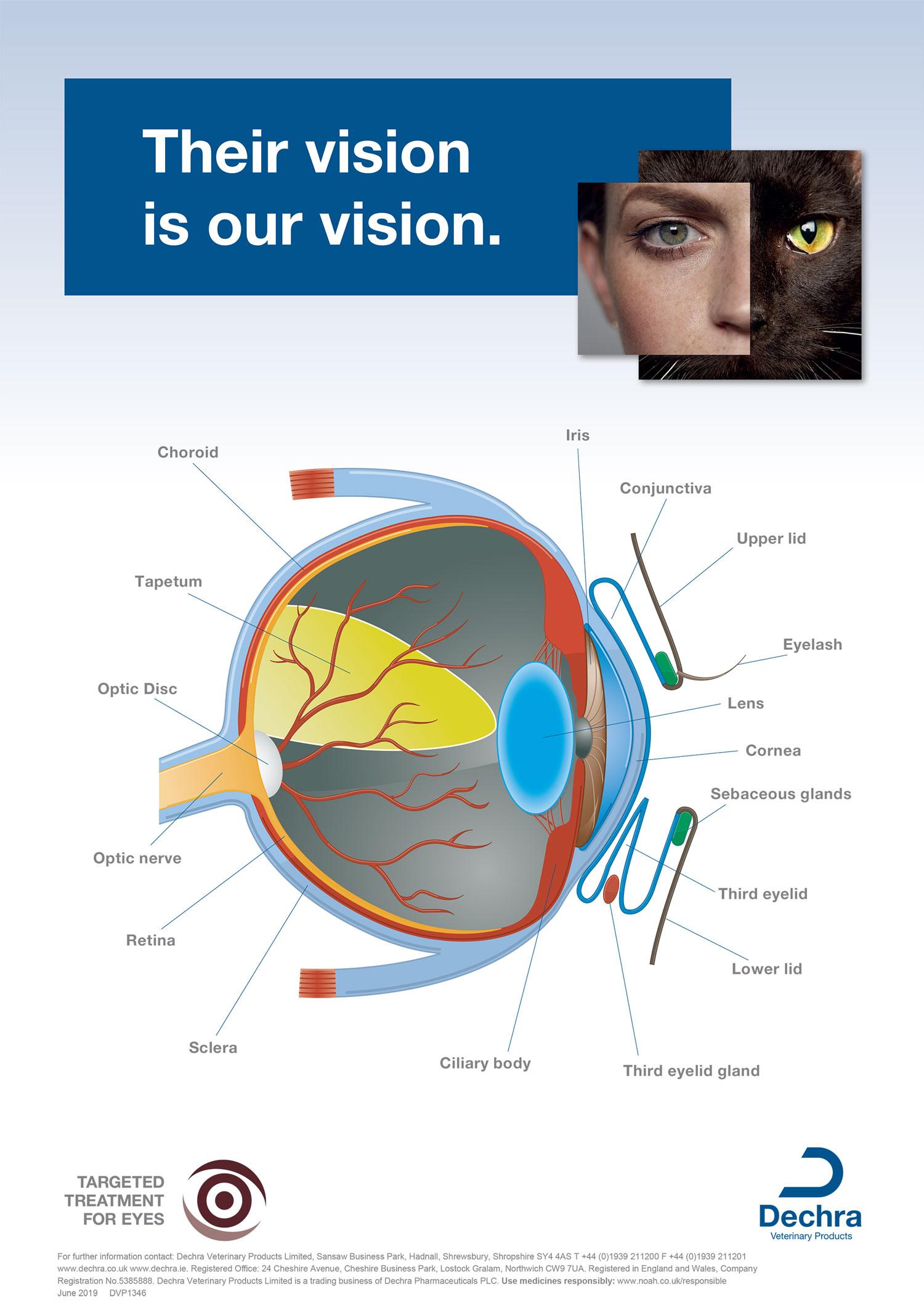
The uveal tract is the term used to describe the vascular, middle layer of the eye. It has three parts:
The Iris
The iris works to vary the size of the pupil and therefore controls the amount of light which enters the eye. To do this, the iris has two sets of muscles; the sphincter muscle, which encircles the pupil and constricts the pupil, primarily through parasympathetic innervation, and the dilator muscle, whose radially orientated fibres allow for pupil dilation, predominately through sympathetic innervation.
The Ciliary Body
The ciliary body sits behind the iris and in front of the choroid. As described in the Aqueous section, it is important in ocular metabolism - playing a large role in the production and drainage of the aqueous. It also helps to suspend the lens, and therefore plays a smaller role in accommodation of the lens.
Choroid
The choroid can be found in between the sclera and the retina and is a highly vascularised structure, which helps to provides blood to the outer retina. A reflective layer, known as the tapetum, sits within the choroid and works to reflect light back through the photoreceptors - increasing visual sensitivity.
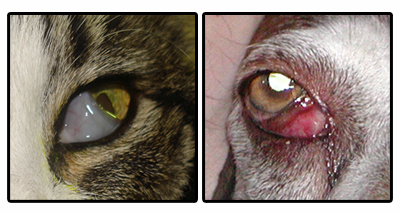
The uveal tract plays a key role in maintenance of the blood-aqueous barrier and disease of its structures can cause a breakdown of this barrier.